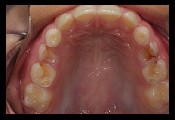
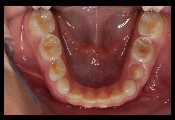
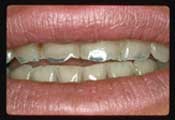
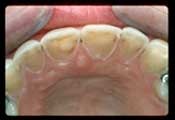
Erosive tooth wear may be diagnosed by integrating a review of findings from a detailed health history, assessment of relevant risk factors, and a comprehensive clinical examination.1 The process of erosive tooth wear begins with initial softening of the enamel surface with subsequent and/or progressive loss of volume, with a softened layer (i.e., less surface hardness) remaining at the mineralized tooth surface.47 Individuals with erosion may also present with dentition that has loss of enamel texture and/or a silky, glossy or “melted” appearance, with cupped, flattened or smoothed occlusal surfaces (or without the sound morphology of natural dentition).1, 27,48
A detailed health history-taking process can help identify high-risk conditions (e.g., GERD, bulimia) or underlying causes that can elevate risk of exposure to acid erosive challenges, primarily acids of intrinsic (gastric) or extrinsic (dietary) origin. In the oral examination, the dentist may observe common signs of erosive tooth wear, such as shallow defects (typically on smooth surfaces) and cupping or flattening on occlusal surfaces (examples presented in photos in the “Gastroesophageal reflux” section above).1 Additional signs of progressive erosive tooth wear may include dentin hypersensitivity and/or erosive lesions with absence of staining.27, 49 Early diagnosis of dental erosion can be challenging because patients often present without clear or clinically evident symptoms.27
Since dental erosion results in progressive and irreversible loss of mineralized tooth substance, the primary focus of erosion intervention is prevention and reduction, followed by management.17 Clinical management typically includes lifestyle and dietary changes, and, if necessary, restorative treatment to halt progression of erosive lesions.17, 50
Some studies have found that milk and yogurt products (presumably unsweetened) may have a protective effect against erosion13, 17, 40 hypothesized to be due to their calcium and phosphate content.40 While calcium supplemented to acidic beverages, and other calcium-enriched products, have been suggested as protective alternatives to soft and sports drinks,17, 40 the efficacy of this strategy has not been thoroughly investigated. Fluoride may contribute to remineralization of enamel,9, 51 but others have advised that fluoride’s “ability to prevent erosion cannot be presumed.”3
More recently, however, several in situ studies52-59 suggest that fluoride treatments are effective in protecting dental enamel from the effects of erosion, although efficacy varies according to compound or preparation, and further research is needed.