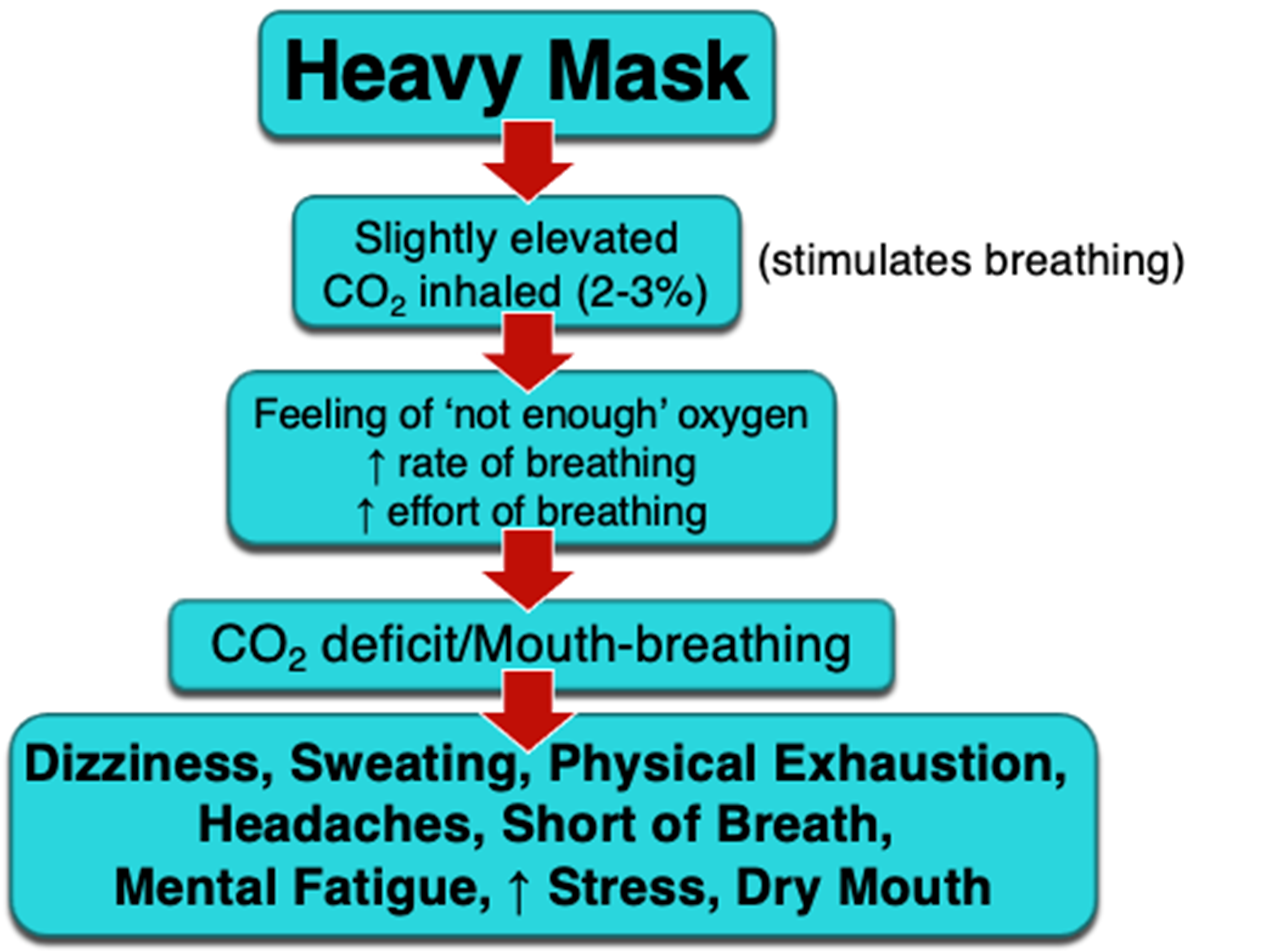
Sweating, visual changes, headache, dyspnea, increased irritability, and decreased reasoning, alertness, and exercise endurance can result.2 A question that often arises is, “is this damaging my health”? Multiple N95 studies show that in spite of the increased CO2 levels, and subjective discomfort complaints, there was no “clinically relevant physiologic burden or damage in the subjects.” 4,5 (Ozdemir, Rebmann)
Nevertheless, these symptoms of heavy mask wearing are not comfortable, and they are exacerbating the (already problematic) incidence of work-related physical pain among dentists. My research revealed that a lot can be done to mitigate these symptoms by integrating several evidence-based techniques in the operatory.
One of these is the manner in which you breathe in the operatory. Consider nose versus mouth breathing: with nose breathing, you have the natural defense of nitric oxide in the nasal cavity which has anti-viral properties and can defend against respiratory tract infections. Mouth breathing offers no protection against inhaled elements in the air, and causes a 42% water loss compared to nose breathing. This can lead to dehydration, thirst and overheating.
So is nose breathing the answer to the adverse effects that dental professionals are experiencing with heavy PPE: headaches, exhaustion, dehydration, decreased cognition and dizziness? The answer is a resounding NO! It is the manner in which you nose breathe that can increase or worsen these symptoms. I am not referring simply to chest versus abdominal breathing, but ‘Relaxed Breathing’ versus ‘Stress Breathing.’
Stress breathing is fast, shallow, done through the mouth upper chest. On the other hand, relaxed breathing is slow, deep, soft and done through the nose and abdomen. The below exercise will help you become aware of how you can easily implement relaxed breathing in the operatory to decrease headaches, dehydration, dry mouth, decreased cognition and physical exhaustion.
Exercise
Place one hand on your stomach and imagine your lungs divided into 4 parts, from the bottom up.
As you inhale, think of three things:
- Breathe in deeply, into your lower abdomen, filling the area under your hand.
- Breathe in softly that you can’t even hear the action occurring.
- Breathe in slowly, only 6 breaths per minute.
Now inhale and fill the lower ¼ of your lungs, and hold for 4 counts. Inhale again and fill the next ¼ of your lungs, and hold for 4 counts. Inhale again and fill the next ¼ of your lungs and hold for 4 counts. With the last breath, you will fill your entire lungs, and hold for 4 counts.
Repeat the process for exhaling.
You will find this exercise activates your parasympathetic nervous system (relaxation response), which can dramatically reduce the negative impact of heavy PPE in the operatory!
References
- Guignon A. Headaches, exhaustion, anxiety: The physical and emotional challenges of returning to work during the pandemic 2020.
- Davis B., Tsen L. Wearing an N95 Respiratory Mask An Unintended Exercise Benefit? Anesthesiology 2020 Sep;133(3):684-686.
- Matuschek C. et al. Face masks: benefits and risks during the COVID‑19 crisis. Eur J Med Res. 2020 Aug 12;25(1):32.
- Ozdemir L, Azizoglu M., Yapici D. Respirators used by healthcare workers due to the COVID-19 outbreak increase end-tidal carbon dioxide and fractional inspired carbon dioxide pressure. J Clin Anesth 2020 Nov;66:109901.
- Rebmann T, Carrico R., Wang J. Physiologic and other effects and compliance with long-term respirator use among medical intensive care unit nurses. Terri Rebmann J Infect Control 2013 Dec;41(12):1218-23.